
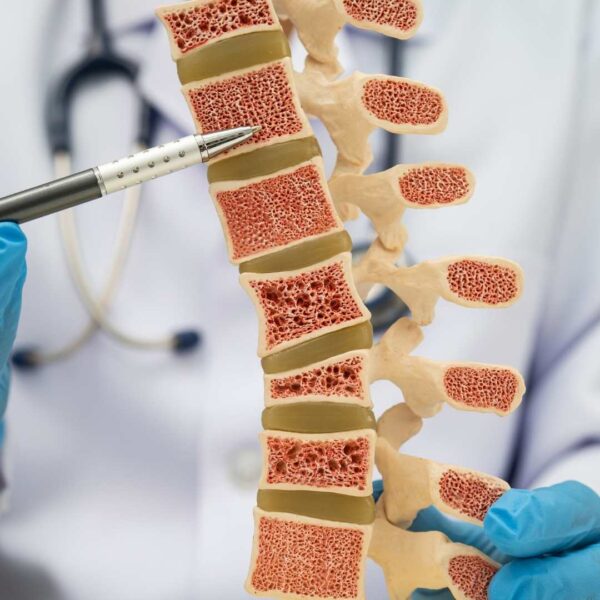
Dual-energy X-ray absorptiometry, or DXA (previously known as DEXA), is the most widely used method of measuring bone density. Other tests such as CT scans, dual photon absorptiometry, and ultrasound may also estimate bone density but are less common. DXA scan results are typically the first step to get an osteoporosis or osteopenia diagnosis.
What Is A DXA Scan?
Dual-energy X-ray absorptiometry, or DXA, also called bone densitometry, is a specialized form of X-ray technology. Whereas a traditional X-ray can visualize bone fractures but has limited ability to estimate bone density, DXA scans are designed to measure bone mineral density (BMD). As a result, medical professionals use DXA scans to diagnose osteoporosis, osteopenia, and other conditions that affect bone density. A newer application of DXA scans includes estimating body composition, such as body fat. But the most common use of a DXA scan is to measure bone density.
Physicians typically recommend that post-menopausal women undergo DXA scans to obtain bone density measurements. For individuals with certain risk factors – for example, those who take medications that are known to cause bone loss (such as glucocorticoids, to name one) and those with a family history of osteoporosis, doctors typically recommend scans at a younger age.1
Synopsis
DXA scans provide a measurement of bone density that doctors use to diagnose osteoporosis and osteopenia.
Types of DXA Machines
There are two types of DXA machines: central and peripheral. In most cases, physicians request DXA scans of the lower spine and hips, performed using a central DXA scanner.
In some cases, such as when evaluating bone density in children, the entire body may be scanned. Unlike other forms of imaging, such as CT scans or MRIs, a DXA scan does not require to be placed in a “tunnel” or enclosed space. Instead, a central DXA device looks like a flat, padded table with an arm extended above the patient.
In other cases, a peripheral DXA scanner may be used to conduct bone density screening. Peripheral DXA scanners are more portable, making them suitable for mobile medical units and other applications where portability is essential. These scanners look like a box with space allowing to insert a foot or hand. Peripheral DXA scanners can measure bone density of the wrist, finger, or heel.
Synopsis
There are two major types of DXA machines, central and peripheral, each of which has its own benefits and drawbacks.
Stronger Bones. Without Drugs. Guaranteed!
The natural and evidence-based program that helps reverse osteoporosis and osteopenia in 12, 6, even 3 months… guaranteed.

How Does A DXA Scan Work?
During a DXA scan, the machine aims two X-ray beams at the patient’s bones. Each X-ray beam has a different energy level. Because healthy bone tissue is dense and rich in minerals, it blocks a large number of the X-rays. This means that relatively little X-ray energy reaches the detector on the other side of the scanner. For individuals with lower bone density (i.e., less mineralization), more of the X-rays penetrate the bone tissue.2
Using two X-ray beams of different energy levels improves the accuracy of resulting bone density measurements. One of the X-ray beams has a peak absorption by soft tissue, while the other has peak absorption by bone. When the signal from soft tissue is subtracted, the DXA scan provides a measure of average bone density.
Synopsis
DXA scans measure how X-ray energy penetrates bones. The less dense the bone tissue, the greater the X-ray beams penetration.
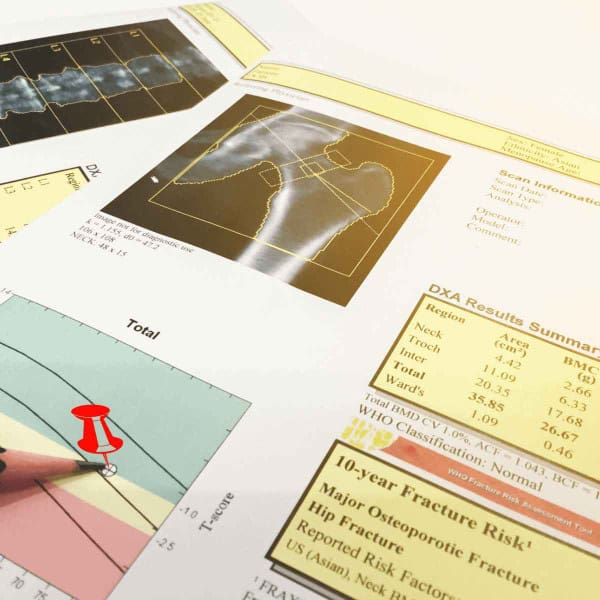
How To Interpret A DXA Scan
After the scan is complete, a radiologist reviews the scan. Once the radiologist analyzes the results, he or she sends a signed report to the referring doctor.
DXA scans offer multiple scores for the physician to interpret. The primary output is a measurement known as Bone Mineral Density (BMD). This may be expressed by two primary types of scores:3
T-score: the T-score is the primary score yielded by the DXA scan. It compares bone density to that of a typical 30-year-old (the age of peak bone density). T-scores are expressed in units of standard deviations (SD) from the mean. Thus, a T-score of -1.0 indicates that your bone density is 1 standard deviation below the mean of a 30-year-old. In general, T-scores are interpreted as follows:
A T-score of or above -1.0 indicates normal bone density.
-1 to -2.4 suggests mildly low bone density or osteopenia. This condition is sometimes called “pre-osteoporosis.”
Scores at -2.5 and below indicate osteoporosis. Thus, people diagnosed with osteoporosis have a bone density score that is at least 2.5 standard deviations below the mean.
Z-score. The DXA scan also provides a Z-score, which adjusts for age and sex. Again, according to the guidelines, low scores reflect poorer bone density while higher scores indicate greater bone density.
Synopsis
All DXA scans result in easy-to-interpret numbers that measure bone density. The bigger the number (i.e., more negative), the lower the bone density.
The Arbitrary Nature Of Measuring Bone Density
Despite the widespread use of DXA scans, the above guidelines were arbitrarily created back in 1992 during a conference in Rome sponsored by the World Health Organization (WHO) and the International Osteoporosis Foundation (IOF).
Read this article to get all the details on how and why this happened:
One issue is that the reference group used to measure bone mineral loss considered to be the “norm” is the Standard Peak Bone Mass, measured in a group of younger adults in their late 20s.4
Bone mineral density measurements are compared to this normative group to derive the T-score and Z-score. However, there are no international standards for Peak Bone Mass, as bone density varies by ethnicity and geographic location.
Another downside of bone density measurements is the lack of clear evidence linking bone mineral density with fracture risk. Diagnosis of osteopenia, or “pre-osteoporosis” is widespread among older adults, yet it is unclear whether mildly low bone mineral density levels make fractures more likely.5 Relying solely on a DXA scan to diagnose osteoporosis or osteopenia ignores other relevant risk factors, including age, height, weight, gender, ethnicity, smoking status, taking glucocorticoid medications, family history, diet, exercise, and other lifestyle variables.
Additionally, DXA scan results do not include a crucial measurement of bone health: tensile strength. As explained in the Osteoporosis Reversal Program:
“Tensile strength is the ability of a material or member to resist stretching and pulling, and is different from compressive strength. The latter means that a material or member has the ability to resist compression or crushing… Bone compressive strength is always much greater than tensile strength; tensile strength must therefore be of primary concern.”
Synopsis
There is a lack of scientific consensus about the interpretation of bone density measurements in regards to risk of fracture. Additionally, DXA scans do not measure tensile strength. Taking a holistic view of health is more accurate than relying on a single number from a DXA scan.
Bone Quantity Versus Bone Quality
Physicians use DXA scans as a diagnostic tool for osteoporosis and osteopenia because they provide a score that determines whether someone falls in the “normal” range or “osteoporosis” range. Unfortunately, this approach ignores the difference between bone quantity and bone quality. Bone is living tissue made up of minerals and collagen woven into a complex matrix.
When new bone grows during puberty, bone formation rapidly outpaces bone loss. Eventually, however — typically in the mid to late 30s, the rate of bone resorption outweighs creation of new bone tissue.6 This is due to normal biochemical changes that alter the activity of osteoblasts (cells that build bone) and osteoclasts (cells that tear down bone).7 The process accelerates for women after menopause due to changes in hormonal levels.
The take-home message is that to prevent fractures, bone quality is more important than bone quantity. Following a pH-balanced diet, consuming the Foundation Supplements, exercising to build density and get fit, and maintaining a healthy lifestyle has been shown improve the overall quality of our bones. Unfortunately, that is something that cannot be reflected by DXA scan results, which measure only bone quantity.
Synopsis
Don’t rely on a single measurement of bone density. When it comes to fracture prevention, quality, rather than quantity, of bone tissue is more important.
Are DXA Scans Accurate?
The inaccuracy of DXA scans also remains a significant concern for patients and care providers. In a 2001 study published in the Osteoporosis International journal, participants underwent scans in three different scanners made by different manufacturers.8 Even when using specialized equations to account for differences between the DXA scanners, intra-individual measurements differed by an average of 3.5%. Thus, getting a DXA scan on one machine may result in a “normal” scan, while a scan on the same day in a different scanner might lead to a diagnosis of osteopenia.
These findings present an additional challenge for those who would like to track their bone mineral density over time because they would need to repeat scans on the exact same scanner every time. Otherwise, results may vary so much as to be meaningless.
The poor reliability of the DXA procedure makes it challenging to interpret results, casting doubt on osteoporosis diagnoses made solely based on DXA scan results.
Synopsis
Scanner differences and poor reliability make DXA scan results error-prone.
Take-Home Message
Although DXA scans provide a snapshot in time regarding your bone density, results have poor accuracy, arbitrary measurements, and do not reveal bone quality. Unfortunately, this has led to a significant osteoporosis and osteopenia over-diagnosis in the United States and around the world. A growing body of evidence suggests that these bone density measurements do not clearly correlate with outcomes such as fracture risk.
Focusing on a natural, holistic approach to bone health has been shown to reverse osteoporosis and osteopenia, improve bone quality, and reduce the risk of bone fractures.
References:
1 1. Jeremiah, M.P., Unwin, B.K., Greenawald, M.H., and Casiano, V.E. “Diagnosis and management of osteoporosis.” American Family Physician. 2015. 92:261-268.
2 Berger, A. “How does it work? Bone mineral density scans.” British Medical Journal. 2002. 325:484.
3 American Bone Health. “Understanding Bone Density Results.” Web. https://americanbonehealth.org/about-bone-density/understanding-the-bone-density-t-score-and-z-score/
4 National Institutes of Health Osteoporosis and Related Bone Diseases National Resource Center. “Bone Mass Measurement: What the Numbers Mean.” Web. https://www.bones.nih.gov/health-info/bone/bone-health/bone-mass-measurement-what-numbers-mean
5 Marshall, D., Johnell, O., and Wedell, H. “Meta-analysis of how well measures of bone mineral density predict occurrence of osteoporotic fractures.” British Medical Journal. 1996. 312:1254.
6 Demontiero, O., Vidal, C., and Duque, G. “Aging and bone loss: new insights for the clinician.” Therapeutic Advances in Musculoskeletal Disease. 2012. 4:61-76.
7 Chan, G.K. and Duque, G. “Age-related bone loss: old bone, new facts.” Gerontology. 2002. 48:62-71.
8 Lu, Y., Fuerst, T., Hui, S., and Genant, H.K. “Standardization of bone mineral density at femoral neck, trochanter and Ward’s triangle.” Osteoporosis International. 2001. 12:438-444.








Hi vivian ,
I am a member and i ordered all your books.i can’t log in to customer support. How can i email or ask questions.?..
Vivian, I am so happy that a good friend of my introduced me to your program after being on fosamex for 5 years – and declining in bone density anyway. My dr wanted me to have an infusion – thankfully I did not and try to follow the program. I am also a fitness enthusiast and workout 4 to 5 times a week. While I try to not focus on bone density scores, it’s hard to ignore decline.My 1st Dexa scan following start up of your program 4 years ago showed decline (below -2.5) but “not significant.” My latest dexa however showed “significant decline” and I am now at -3.0. At what point should I be worried? (As I already am….) What am I doing wrong?
Being a registered nurse for 27yrs with a master’s degree in adult care and administration, (and continue to work) my GYN physician attempted to recommend a bone therapy drug regiment after reading my DXA results approximately 5 yrs ago. When I questioned him what did he think about the horrible side effects of the drugs and that the drugs he was suggesting were basically bone hardeners (which put the individual in more risk of fractures), not actually allowing the calcium to retain in the bone itself in order to produce healthier bone material; well he didn’t have much to say. Again, I give much thanks to all of the research you provide. We do listen.
Thx so much Vivian for the continuous research of information you have provided throughout the years. I’ve learn so much. Keep of the good work.
Hi there,
My husband had a DXA scan in 2015 and it showed osteopenia. Had another DXA in 2016 and his osteopenia result had stayed the same. Just had another DXA scan and it showed that he is now in osteoporosis. He is a healthy 46 year old male who works out and doesn’t drink or smoke and this should not be happening. Blood work is great and his calcium is fine. The two endocrinologists that we saw couldn’t figure out why. We finally saw a specialist and they said it could be related to environmental exposure. Is this a thing? Any information would be helpful.
I just found this site & have already learned important information. I’d like to join. Thank you.
What do you know about Tymlos? Just got home from a consultation with a lady who specializes in osteoporosis. My bones are real bad and she gave me the big scare routine. Tymlos is the newest on the market. I do have 4 compression fractures. What would you do? I am against these drugs. I know alkaline food is the way to go but I need to gain weight.
Nancy, don’t fall prey to scare tactics! At the Save Institute we never recommend taking osteoporosis drugs. You can read our previous article on Tymlos here:
https://saveourbones.com/the-truth-about-tymlos-abaloparatide-the-newest-osteoporosis-drug/
And you can gain weight while on a pH-balanced diet. For example, focus on consuming a good amount of calories from alkalizing foods, such as sweet potatoes, potatoes, quinoa, white beans, avocado, almonds, and sunflower seeds (to name a few).
You can also make smoothies, adding your favorite nut butter. Here are a few recipes to get you started:
https://saveourbones.com/digestive-troubles-try-these-3-smoothies-that-aid-digestion-alkalize-your-ph-and-boost-absorption-of-bone-building-nutrients/
I don’t have access to my list of alkaline and acidic foods right now as they are in storage but I thought beans were acidic, or are the white beans you mentioned not the white beans I’m thinking of, northern, navy, pea etc.
I recently had a Dexa Scan and the results showed my T-score was lower than the previous scan. However, my results from blood work shows my calcium level is normal. Can you comment on the relationship between calcium levels and bone density?
98% to 99% of calcium is stored in our bones, and there’s a very tight control over the amount of calcium circulating in the blood by parathyroid hormones and Vitamin D. Studies have shown that postmenopausal women have lower serum calcium levels . Here’s one study that explains this:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5661842/
Thank you for the information about the DXA scan.
You’re welcome, Shula!
It would help me greatly if the program I purchased from you was on a DVD.
Is there a way you would offer this.
Karen Heidinger
Karen, we will reply to you via email within the next 24 hours.
Does rheumatoid arthritis change the equation? I am a previously very active 59 year old with RA for 5 years. Thanks to a biologic drug, diet and supplements, I am back to long walks but not my former athletic life. The docs are watching my bone density closely. I’ve been able to fend them off with the meds, but my last DEXA left them thinking that I really need to go this route. Any thoughts?
Therese, RA is certainly a challenge, and it seems you’re on the right track.
At the Save Institute, we never recommend taking osteoporosis drugs, and we are fully aware that most doctors will prescribe them and try to convince their patients to take them.
Here are some articles that will help you stand your ground and find a doctor that will be supportive of your decision:
https://saveourbones.com/who-should-you-trust/
https://saveourbones.com/4-inspiring-steps-to-take-control-of-your-bone-health-and-improve-your-life/
https://saveourbones.com/the-top-three-traits-to-look-for-in-an-osteoporosis-doctor/
Many thanks, Vivian. I will check out those articles!
I have noticed a change of emphasis on your recommenced use of calcium and D3. Am I correct?
Rob, please check your inbox within the next 24 hours. One of our Customer Support agents will address your question and email you a response.
Thank you for the information on the DXA scans. You only mentioned the CT scan for bone loss but gave no information on that. Is it better than the DXA scan or are they both in the same category?
Donna, you’re very welcome! We did not expand on CT scans because this article is about DXA scans. The latter are most commonly requested by doctors with the purpose of diagnosing osteoporosis or osteopenia. However, a recent study published in the Journal of Bone Mineral Research has found that CT scans are as effective as DXA testing.
This is the link to the study:
https://www.ncbi.nlm.nih.gov/pubmed/29665068
Thank you, Ita.
You’re welcome!
Thank you Vivian for this in depth and easy to understand summary on the DXA scan. According to the DXA scan I have had osteoporosis for 4 years (postmenapausal). I also had the urine test NTX telepeptide which put me at 37 which is normal. I am a very active 60 year old and I totally agree with your suggestions about taking the natural approach of diet, exercise, sleep, and supplements to keep my bones strong and healthy. Does the Densercise program offer strength training, such as weights and resistance bands? I already purchased the nutritional programs and love them. I have received 3 reclast treatments and will not do it again. Keep educating us and thank you for your passion !!
Renee
So glad you find today’s article useful and educational, Renee! And we commend you on deciding to not continue with the Reclast infusions.
To answer your question, the Densercise Epidensity Training System does not require the use of any equipment. You can read more about it here:
https://saveourbones.com/densercise/