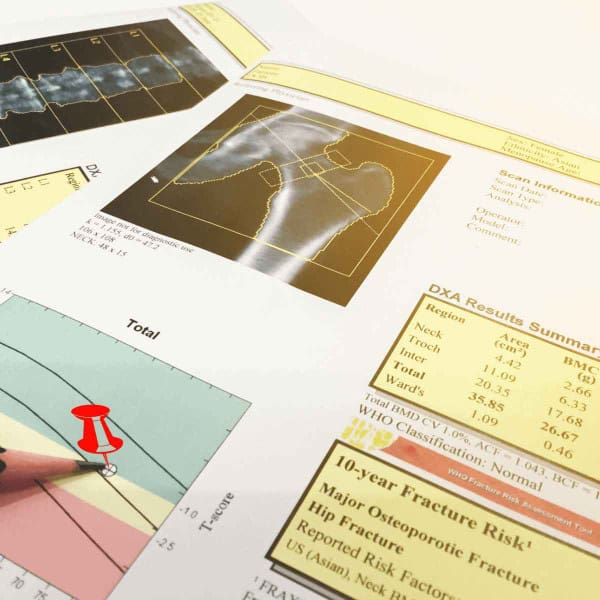
The Medical Establishment relies on bone mineral density (BMD) to assess bone health, diagnose osteoporosis and osteopenia, and prescribe drugs. But there’s more to bone health than just density. For example, there are tests that can measure the bone remodeling process by assessing bone turnover markers (BTM).
Today you’ll learn about bone turnover markers, what they indicate, and which BTM tests provide the most accurate and useful results for assessing the health of your bones.
All About Bone Turnover
In the process of bone turnover cells called osteoclasts dissolve discrete portions of bone, transferring minerals like calcium and magnesium from the bone tissue into the blood. That part of the process is called resorption. Then, cells called osteoblasts replace the dissolved bone with new material. Osteoclasts and osteoblasts work in turn to remove old, damaged bone and then replace it, resulting in strong bones that are in a continuous process of renewal.
When this cycle falls out of balance, the quality of bone is reduced. When osteoclasts outpace osteoblasts, it causes a loss of bone mass and with it a loss of the structural quality of bone.
The opposite problem can also occur, in which osteoblasts outpace osteoclasts– resulting in new bone deposited over old and damaged bone. This can lead to atypical fractures like those caused by many osteoporosis drugs. Ironically, those drugs are prescribed to prevent fractures, but by unbalancing bone turnover, they can cause fractures.
However, the overall rate of bone turnover is also a factor that impacts the strength and quality of bone. The material that osteoblasts deposit into the pits left by osteoclasts takes time to reach full strength and integration into the existing bone. With excessive bone turnover, a larger-than-ideal percentage of bone becomes comprised of this new material. That results in weaker bones.
Conversely, insufficient bone turnover can leave old and damaged bone material for too long. The microcracks that accumulate in old bone eventually jeopardize their structural strength.
Synopsis
Cells called osteoclasts dissolve portions of bone, resorbing minerals into the blood. Then osteoblasts add new bone material. This process of bone turnover keeps bones strong. When it falls out of balance, bone quality is compromised, increasing fracture risk.
Bone Turnover Markers
The rate and balance of bone turnover impact the quality and strength of bones, implicating fracture risk. In fact, bone turnover has been shown to predict fracture risk independently of bone mineral density. This suggests that bone turnover may be a better tool for gauging bone health and fracture risk than bone mineral density alone.1
Researchers have identified compounds and enzymes that appear in the blood or urine as a result of bone turnover. By testing for these bone turnover markers, we can get a snapshot of bone turnover activity. There are two steps in the bone turnover process: resorption and formation. Each step produces unique markers that can be measured with varying levels of accuracy.1
Synopsis
Bone turnover levels predict fracture risk independently of bone mineral density, making it an important tool for assessing bone health. We can measure bone turnover by testing for levels of bone turnover markers, which occur as byproducts of bone resorption and formation.
Bone Resorption Markers
The markers of bone resorption include enzymes involved in the process of bone resorption and the material generated through resorption. There are four categories of bone resorption markers.1,2
- Collagen degradation products are a class of bone resorption marker generated when the collagen in bones is broken down during the resorption process. Their presence and levels in blood or urine indicate how much bone resorption is occurring. This kind of marker includes telopeptides of Type 1 collagen that are C-terminal (CTX-1) and N-terminal (NTX-1).
- Noncollagenous proteins include bone sialoprotein. This glycoprotein stimulates osteoclast-mediated bone resorption and can be measured in blood serum.
- Osteoclastic enzymes are secreted by osteoclasts to break down bone matrix proteins. The two we can measure are tartrate-resistant acid phosphatase and cathepsin K.
- Osteocyte activity markers can also be observed to measure resorption levels. These include RANKL (Receptor activator of nuclear factor kappa-B ligand), osteoprotegerin, and sclerostin. These compounds all play a role in bone resorption, and you may recognize them from osteoporosis drugs. Some drugs artificially limit bone resorption by inhibiting the function of these compounds.
Synopsis
Markers of bone resorption include collagen degradation products, non-collagenous proteins, osteoclastic enzymes, and osteocyte activity markers.
Bone Formation Markers
The other part of the bone turnover process, bone formation, also leaves behind byproducts that we can measure in the blood and urine. Their presence allows us to assess levels of bone formation.
There are three categories of bone formation markers.1,2
- By-products of collagen synthesis are observable in the blood serum. These are propeptides of Type 1 collagen, C-terminal: P1CP and N-terminal: P1NP.
- Osteoblast enzymes include alkaline phosphatase (ALP). This enzyme is present in most body tissues, so it can be measured in total or in its bone-specific form.
- Matrix proteins include Osteocalcin (OC). Osteocalcin is a non-collagenous protein synthesized by osteoblasts. It makes its way into the bloodstream but only survives there for about five minutes before degrading.
Synopsis
Bone formation markers include by-products of collagen synthesis (notably P1CP), osteoblast enzymes, and the matrix protein osteocalcin.
Most Reliable And Useful Bone Turnover Marker Tests
All of the bone turnover markers (BTM) listed above can be measured. However, the accuracy and ease of measuring them vary widely. There are only two BTM tests we recommend, one that measures bone formation, and one that measures bone resorption.
For bone formation markers, a collagen synthesis by-product has proved the most stable and accurate measurement. Procollagen Type 1 N propeptide (P1NP) has proved a consistently accurate measure of bone formation, with minimal variation in accuracy between individuals. Tests measuring P1NP are also reliable.1,2
For resorption markers, C-terminal telopeptide (CTX) measurement is ideal. Specifically, the sCTX1 test has proven most reliable and accurate.1,2 It does vary with circadian rhythms, which results in level peaks in the early morning hours and lows in the afternoon. A practitioner should be aware of this variation.
Synopsis
The Save Institute recommends a Procollagen Type 1 N propeptide (P1NP) test for bone formation and the C-terminal telopeptide, sCTX1 test for bone resorption.
What This Means To You
Add bone turnover marker tests to the clinical assessment tools your doctor can help you use. DXA scans provide a limited view of your bone health. BTM tests can be conducted more frequently and can provide an additional indicator of the health of your bone turnover.
By adding more information to your self-assessment, you can get a broader view of your bone health.
The Osteoporosis Reversal Program takes a holistic approach to bone health– one that includes all of the factors impacting your bones and well-being. That broad approach encompasses bone turnover, bone density, and other factors– such as muscle strength, eyesight, and balance– that impact fracture risk.
When you see the big picture, you can see more paths to the future you deserve.
References
1 https://journals.sagepub.com/doi/pdf/10.1177/0004563213515190







Hi ! Just saw your post on osteoporosis. My Mom is 71, a diabetic and has developed osteoporosis due to an underlying condition of MGUS- Kappa light chain. Her blood calcium levels are normal. & Her t-score is -3 with high risk of fracture for femur rt & left & L1-L4. She was advised Ibandronate sodium (flurish)-150mg once a mth by the doc. After taking the first dose, she developed fever, chills & severe bone pain as a side effect. The doc first denied it was bcoz of meds & then asked her to stop using it & advised denosumab injection. We have heard that it leads to debilitating & lasting pain while leaving patients prone to recurrent infections & didn’t opt for it. Her alkaline phosphate levels went up from 140 to 169 after single dose of oral ibandronate spdium 150mg. Please suggest if there is a safer alternative.
Unreal information – One can only assume that many of the medical profession are not aware of these clinical findings.
My doctor put me on 1800 mg a day for calcium pills, along with Vit. D3 because I wouldn’t take any osteoporosis medications. After 10 years now, she told me to stop taking them. She wouldn’t tell me why. Said I get enough through my diet. I looked on search & found out though a study that too much calcium pills can cause hardening of the arteries. I also read that taking Vit. K2 with Vit. D3 is good by opening up the arteries. My doctor didnt want me to take K-2. After reading medical advice from Harvard health, Mayo Clinic , etc.
I made the decision to take K-2.
I now have found a new doctor. Please explain why you think my doctor would not tell me more on what is going on. I found out she recenty retired at a young age by the way. Which gives me “red flags’.
Unfortunately, many doctors don’t keep up with the latest research. Take a look at this article that delves into this topic:
https://saveourbones.com/the-unfortunate-divide-between-doctors-and-medical-science/
A friend of mine takes 2 to 3 tablespoons of plain gelatin a day in tea or a smoothie or in his oatmeal. He claims it will improve his joints, tendons, ligaments, and increase bone density. Is all this possible? Thanks for your time and wonderful website.
Mary, gelatin is derived from collagen taken from animal body parts and it plays a critical role in bone and joint health. You can read more about this here:
https://saveourbones.com/how-collagen-strengthens-your-bones-and-how-to-support-it/
Do you have comments from people with osteoporosis levels that improved significantly by following this program? Thank you for all the information.
Indeed we do, Maria. Here’s the link to our testimonials page:
https://saveourbones.com/testimonials/
This is really interesting. Next time my doctor recommends biphosphonates, I’ll ask for these tests to be done rather than relying on the results of DEXA scans.
That’s a good move on your part, Jenny 🙂
Where can I get the test you mention in this article BTM, P1CP, P1NP
Thank you’
Miriam
Hi Vivian,
The info you give is so good.
I have had a hip repair mths ago and give days ago I slipped on water and I have, I feel, fractured my sacrum. Please tell me how I can improve my bone strength. I am seeing the Gp tomorrow, but I’m not to happy with myself😢
Thanks for your kind words, Hazel! Diet, exercise, and certain lifestyle habits (as explained in the ORP) are effective ways to improve bone strength.
Thanks for the Bone Marker information. My doctor had the P1NP and CTx test done at my insistence, some doctors do not see any use for them. I (87years) have had a wrist fracture, and bi-lateral insufficiency sacral fractures in the past 2 years so started Tymlos. I continue to exercise and eat well. I am helped by the information on your web site.
My pleasure, Faye! And I thank you for sharing your story with our community.
And this article contains information on Tymlos, in case you missed it:
https://saveourbones.com/the-truth-about-tymlos-abaloparatide-the-newest-osteoporosis-drug/
Thank you, Vivian, for all you do!
Where can one get these tests you’ve just referenced? And are they expensive?
Thanks,
Elisabeth
You’re very welcome, Elisabeth! You can request these tests from your PCP. And pricing is a complex topic since it depends on the health insurance plan you have, the laboratory that will do the tests, etc. I suggest you ask your health insurance company.
R the bone marker tests u hv recommended blood tests or standalone tests like the DXA scan?
For some markers it’s a urine test and for others a blood test.
Hello,
Thank you for all that you do. Some time ago you suggested True Osteo supplements. Currently is this still your recommended supplement?
You’re welcome, Mary! And our supplement recommendation has not changed.