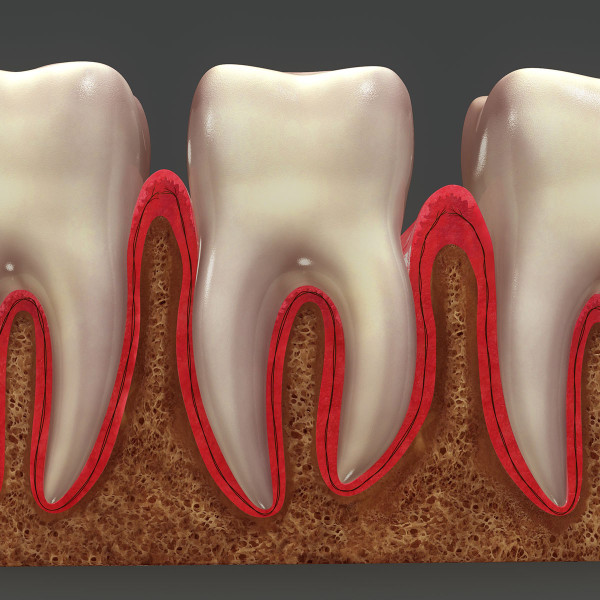
Periodontal disease, also known as gum disease, is an inflammatory process that results in the loss of gum tissue and the alveolar bone that contains the tooth sockets. Without proper dental hygiene, bacteria begin to accumulate on and around the teeth, and the gums become inflamed and weakened.
If unaddressed, this inflammation can cause the deterioration of both the gums and the bones that support the teeth.
Researchers have established links between the inflammation and bone loss caused by periodontal disease and osteoporosis. Not only is there a risk association between the two conditions, but they share a common treatment: an anti-inflammatory diet.
Causes Of Periodontal Disease
Periodontal disease is mainly caused by oral bacteria that secrete a byproduct called plaque. As plaque builds up on the teeth, it causes inflammation in the surrounding gums. If plaque is left on the teeth for too long, it will begin to layer and harden into tartar, which is much more difficult to remove.1
The initial inflammation of the gums is called gingivitis. If the inflammation in the gums increases and spreads to the alveolar bone and teeth, it will eventually lead to loss of gum tissue, bone, and loose or lost teeth. This more severe stage is known as periodontitis.
Both gingivitis and periodontitis are stages of periodontal disease.
Synopsis
Bacteria in the mouth cause periodontal disease by depositing plaque on the teeth that begins a process of inflammation that ultimately causes deterioration of gums and dental bone.
The Links Between Periodontal Disease And Osteoporosis
It was not until 1960 that medical researchers began to suggest a connection between osteoporosis and periodontal disease. Once the comparison began, and as more research emerged about the causes of osteoporosis, it became clear that the two conditions have a great deal in common:
- Both are characterized by bone loss2
- Both commonly affect middle-aged and elderly women.1
- Both share risk factors, including tobacco use, nutrition, age, gender, and menopause.1,2,3
- Both are associated with elevated levels of C-Reactive Protein, a major inflammatory marker4,5
- Both are caused and/or worsened by inflammation4,5
- Both are preventable and reversible through dietary and lifestyle changes6,7
We’ll look at those dietary and lifestyle changes in just a moment. First, we need to understand why those approaches are effective, and the common cause they address.
Stronger Bones. Without Drugs. Guaranteed!
The natural and evidence-based program that helps reverse osteoporosis and osteopenia in 12, 6, even 3 months… guaranteed.

Synopsis
Osteoporosis and periodontal disease share a many risk factors and causes, as well as solutions.
Inflammation: Where Osteoporosis And Periodontitis Meet
In the case of periodontitis, inflammation is understood as the primary cause. The body responds to the buildup of bacteria with an inflammatory response. Instead of helping, this response weakens and ultimately deteriorates both the gums and the bone supporting the teeth and holding them in place.
This cause and effect reveals a biological process that the Save Institute has written about extensively, but which the Medical Establishment rarely admits: inflammation causes bone loss.4
Systemic inflammation is a major risk factor for both periodontal disease and osteoporosis. Inflammation directly interferes with the bone remodeling process, increasing bone resorption, resulting in a loss of bone density and quality.
In one study of nearly 5,000 participants, researches found a 73% increase in hip fracture risk among participants with the highest levels of inflammatory markers associated with hip fracture.4 Excessive inflammation has likewise been found to increase the risk of periodontal disease.5
Bisphosphonates, which actually increase systemic inflammation, can also have a devastating effect on the bones of the mouth. Osteonecrosis of the jaw, a condition in which the jaw bone deteriorates, is a side effect of bisphosphonates.
Synopsis
Both osteoporosis and periodontitis are linked to systemic inflammation, which underscores the bone damage caused by inflammation.
Anti-Inflammatory Diet Protects Bone
Since systemic inflammation increases the risk of both periodontal disease and osteoporosis, decreasing inflammation helps to prevent and reverse both conditions.
One highly effective way to reduce your inflammation levels is through diet. Savers who are following the 80/20 pH-balanced diet outlined in the Osteoporosis Reversal Program are already eating foods that naturally reduce inflammation, and reducing the consumption of foods that cause inflammation.
An anti-inflammatory diet offers numerous health benefits, since systemic inflammation has been linked to many undesirable conditions beyond the two we’re discussing today, including:
- Atherosclerosis8
- Heart attack8
- Stroke8
- Diabetes mellitus9
- Obesity9
- High blood pressure10
- Macular degeneration11
- Rheumatoid arthritis12
- Fatigue13
- Depression14
By following an anti-inflammatory diet, not only do you reduce fracture risk and protect your gums and teeth, you reduce your risk of the life-altering conditions listed above.
The association between osteoporosis and periodontitis also opens the question of how the two conditions impact each other. In one review of studies published on this relationship, researchers found that 11 out of 17 studies shows a positive relation between osteoporosis and periodontal disease. The studies indicate that participants with osteoporosis were more likely to lose alveolar bone. For people with osteoporosis, periodontitis is more likely and more severe.2
Synopsis
Systemic inflammation damages bone, both in the case of osteoporosis and periodontitis. Inflammatory markers have also been linked to a variety of other conditions and diseases, ranging from heart attack to obesity, to depression.
Top Anti-Inflammatory Foods
Certain foods are known to increase inflammation, and other foods are anti-inflammatory. By adjusting the makeup of your meals, you can impact inflammation in your body, and support healthy bones, healthy gums, and overall wellness.
Include these anti-inflammatory micronutrients in your diet:
- Vitamin C – This Foundation Supplement, also known as ascorbic acid, has been shown to have a direct correlation to gum health. A study on people with periodontal disease found they had lower Vitamin C levels that participants with healthy gums and a Vitamin C supplement improved their gum disease.15 Vitamin C is a building block of collagen, which comprises 90% of organic bone material. Vitamin C is found in many fruits, vegetables, and leafy greens, including cantaloupe*, cauliflower*, and collard greens*. You can also take a daily Vitamin C supplement of at least 500 mg.
- Zinc – Another Foundation Supplement, zinc is critical for cell growth. A study found that participants with zinc deficiencies were more likely to have periodontal disease.16 Zinc increases new bone formation by enhancing proliferation of osteoblasts and synthesis of collagen. Meats are a rich source of zinc, but it’s also present in plant-based foods, such as spinach*, broccoli*, oats*, nuts, and seeds. We recommend you take 25 mg a day of amino-acid chelated zinc.
- Beta-Carotene – This antioxidant form of Vitamin A has been linked both to decreased hip fracture risk and improved healing of periodontal disease.17,18 Beta-carotene also gives orange fruits and vegetables their color, so add some carrots* and sweet potatoes* to your meals for a boost of this nutrient. You can also take 5000 IUs in supplement form.
- Omega-3 Fats – Maintaining a healthy balance of essential fatty acids helps to improve bone mass density, reduce inflammation, and support periodontal health.19,20 Top sources include fatty fish, flaxseed*, chia seed, cruciferous vegetables, and mangoes.
- Lycopene – Lycopene is a powerful antioxidant and carotenoid polyphenol. Studies have shown that just 4 mg of lycopene daily is an effective treatment for periodontal disease.21 It also protects and stimulates osteoblasts, promoting healthy bone remodeling.22 Lycopene is what gives tomatoes their brilliant red color, and makes the fruit essential for bone and periodontal health. Other lycopene rich foods include guava, papaya and pink grapefruit.* Two tablespoons of tomato puree contains 27 mg of lycopene.
- Fiber – High fiber diets have been shown to reduce inflammation markers, and the same study links fiber to improvements in a periodontal disease marker.23 Other studies show that fiber helps to reduce bone loss, besides reducing inflammation.24
In addition to those mentioned above, here are some particularly effective anti-inflammatory foods. Not all of them are alkalizing, so be sure acidifying foods are contained within the 20% of your 80/20 pH-balanced diet reserved for them.
- Walnuts*
- Fatty fish*
- Extra-virgin olive oil
- Cranberries*
- Broccoli*
- Red Wine
- Red grapes*
- Dark chocolate*
- Green tea
*Foundation Foods
Conversely, below are foods that increase inflammation. These should be avoided or consumed only in moderation:
- Refined grains
- Sugar
- Cooking oils rich in Omega-6
- Dairy
- Animal Protein
- Alcohol
- Trans-unsaturated fatty acids
Synopsis
A diet rich in anti-inflammatory foods and low in inflammatory foods helps to prevent and reverse both periodontal disease and osteoporosis.
The Following Behaviors Are Part Of A Holistic Approach To Health
Dental experts recommend you brush your teeth at least twice a day and to floss daily to remove the plaque buildup from your teeth, thereby avoiding the inflammation response that becomes periodontal disease.
Most dentists recommend brushing with a toothpaste that contains fluoride, but because fluoride damages bone, the Save Institute recommends using an all natural toothpaste or making one yourself.
Here are some other behaviors that can help reduce inflammation to improve bone quality and improve periodontal health alike:
- Don’t take bisphosphonates
- Don’t smoke
- Practice a focused breathing activity like tai chi or yoga
- Practice positivity
- Prioritize getting sufficient quality sleep
- Actively reduce stress
- Get regular exercise
Use the information you learned today to make the best possible decisions for your health. Celebrate the fact that the most effective and positive health choices you can make have multiple benefits across many different body systems. That’s one of the main reasons why a natural, holistic approach to bone health is so much more effective and life-enriching than a pharmaceutical treatment.
Stop Worrying About Your Bone Loss
Join thousands of Savers from around the world who have reversed or prevented their bone loss naturally and scientifically with the Osteoporosis Reversal Program.
References:
1 Maria Angeles Martínez-Maestre, et al. “Periodontitis and osteoporosis: A systematic review.” Climacteric. December 2010. Web. https://www.researchgate.net/profile/Guillermo_Machuca/publication/45535507_Periodontitis_and_osteoporosis_A_systematic_review/links/0046352e63254121bb000000.pdf
2 Esfahanian, Vahid et al. “Relationship between osteoporosis and periodontal disease: review of the literature” Journal of dentistry (Tehran, Iran) vol. 9,4 (2012): 256-64. Web. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3536461/
3 Bhardwaj, Amit and Shalu Verma Bhardwaj. “Effect of menopause on women’s periodontium” Journal of mid-life health vol. 3,1 (2012): 5-9. Web. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3425152/
4 Shinya Ishii, et al. “C-Reactive Protein, Bone Strength, and Nine-Year Fracture Risk: Data From the Study of Women’s Health Across the Nation (S” J Bone Miner Res. 2013 Jul; 28(7): 10.1002/jbmr.1915. WAN). Web: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3880424/
5 Tushika Bansal, et al. “C-Reactive Protein (CRP) and its Association with Periodontal Disease: A Brief Review” J Clin Diagn Res. 2014 Jul; 8(7): ZE21–ZE24. Web: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4149169/
6 Orchard, T., Yildiz, V., et al. “Dietary Inflammatory Index, Bone Mineral Density, and Risk of Fracture in Postmenopausal Women: Results From the Women’s Health Initiative.” J Bone Miner Res. 2017 May;32(5):1136-1146. Web. https://www.ncbi.nlm.nih.gov/pubmed/28019686
7 Postmenopausal Women: Results From the Women’s Health Initiative.” J Bone Miner Res, 2017. 32: 1136–1146. Web: https://onlinelibrary.wiley.com/doi/10.1002/jbmr.3070/abstract
8 Dodington DW, Fritz PC, Sullivan PJ, Ward WE. “Higher Intakes of Fruits and Vegetables, β-Carotene, Vitamin C, α-Tocopherol, EPA, and DHA Are Positively Associated with Periodontal Healing after Nonsurgical Periodontal Therapy in Nonsmokers but Not in Smokers.” J Nutr. 2015 Nov;145(11):2512-9. Web. https://www.ncbi.nlm.nih.gov/pubmed/26423734?report=docsum
9 Moutsopoulos NM1, Madianos PN. “Low-grade inflammation in chronic infectious diseases: paradigm of periodontal infections.” Ann N Y Acad Sci. 2006 Nov;1088:251-64. Web. https://www.ncbi.nlm.nih.gov/pubmed/17192571
10 Genco RJ1, Grossi SG, Ho A, Nishimura F, Murayama Y. “A proposed model linking inflammation to obesity, diabetes, and periodontal infections.” J Periodontol. 2005 Nov; 76(11 Suppl):2075-84. Web. https://www.ncbi.nlm.nih.gov/pubmed/16277579
11 Sridevi Devara, David Siegel, Ishwarlal Jialal. “Statin Therapy in Metabolic Syndrome and Hypertension Post-JUPITER: What is the Value of CRP?” Curr Atheroscler Rep. 2011 Feb; 13(1): 31–42. Web: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3018293/
12 Emina Colak, et al. “The role of CRP and inflammation in the pathogenesis of age-related macular degeneration” Biochem Med (Zagreb). 2012 Feb; 22(1): 39–48. Web: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4062327/
13 Maria I. Danila. “The Role of Genetic Variants in CRP in Radiographic Severity in African Americans with Early and Established Rheumatoid Arthritis” Genes Immun. 2015 Oct; 16(7): 446–451. Web: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4707038/
14 L. L. Carpenter, et al. “C-reactive protein, early life stress, and well-being in healthy adults “ Acta Psychiatr Scand. 2012 Dec; 126(6): 402–410. Web: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3580169/
15 Daly M. “The relationship of C-reactive protein to obesity-related depressive symptoms: a longitudinal study.” Obesity (Silver Spring). 2013 Feb;21(2):248-50. Web: https://www.ncbi.nlm.nih.gov/pubmed/23404927
16 Gokhale NH1, Acharya AB, Patil VS, Trivedi DJ, Thakur SL. “A short-term evaluation of the relationship between plasma ascorbic acid levels and periodontal disease in systemically healthy and type 2 diabetes mellitus subjects.” J Diet Suppl. 2013 Jun;10(2):93-104. Web. https://www.ncbi.nlm.nih.gov/pubmed/23725523
17 Orbak R, Kara C, Ozbek E, Tezel A, Demir T. “Effects of zinc deficiency on oral and periodontal diseases in rats.” J Periodontal Res. 2007 Apr;42(2):138-43. Web. https://www.ncbi.nlm.nih.gov/pubmed/17305872
18 Z. Dai, L-W Ang, W-P Koh. “Dietary carotenoids reduced hip fracture risk in lean men: the Singapore Chinese Health Study”. Osteoporosis Int. 2012 December Vol. 23 Suppl 7
19 Dodington DW, et al. “Higher Intakes of Fruits and Vegetables, β-Carotene, Vitamin C, α-Tocopherol, EPA, and DHA Are Positively Associated with Periodontal Healing after Nonsurgical Periodontal Therapy in Nonsmokers but Not in Smokers.” J Nutr. 2015 Nov;145(11):2512-9. Web. https://www.ncbi.nlm.nih.gov/pubmed/26423734
20 Naqvi AZ, Buettner C, Phillips RS, Davis RB, Mukamal KJ. n-3 fatty acids and periodontitis in US adults. J Am Diet Assoc. 2010;110(11):1669-75. Web. https://www.ncbi.nlm.nih.gov/pubmed/21034880
21 Weiss et al. “Rancho Bernardo Study.” Am J Clin Nutr 81: 934. 2005. Web. https://www.ncbi.nlm.nih.gov/pubmed/24187655
22 Belludi SA, et al. “Effect of lycopene in the treatment of periodontal disease: a clinical study.” J Contemp Dent Pract. 2013 Nov 1;14(6):1054-9. Web. https://www.ncbi.nlm.nih.gov/pubmed/24858750
23 Kim, Rao, Journal of Medicinal Food, “Lycopene II – Effect on osteoblasts”. 2003
24 Kondo K, et al. A high-fiber, low-fat diet improves periodontal disease markers in high-risk subjects: a pilot study. Nutr Res. 2014 Jun;34(6):491-8. Web. https://www.ncbi.nlm.nih.gov/pubmed/25026916
25 Dai Z, Zhang Y, Lu N, Felson DT, Kiel DP, Sahni S. “Association Between Dietary Fiber Intake and Bone Loss in the Framingham Offspring Study.” J Bone Miner Res. 2017. Web: https://www.ncbi.nlm.nih.gov/pubmed/29024045.










Love your articles! They get right to the point and the synopsis is wonderful! Not a lot of medical jargon which can turn people off. You tell it like it is and I appreciate that!! I have both osteoporosis and periodontal disease and your article is giving me hope! I will try to be better about those supplements and eating those foundation foods. Thank you, thank you, thank you for all your advice and help! You are amazing! We are so grateful for all you do!
I have good news! Had my teeth cleaned today and whatever I am doing at home is good! 80 years and using toothpaste without fluoride, No cavities and my teeth feel clean after all that scrapping. My husband helps us eat healthy and we travel in our RV with friends. Thank you for helping me avoid Prolia. My new doctor tries to understand my refusal to try Prolia. I am trying to educate her, she did recommend a wonderful foot doctor, who really trimmed all my ingrown toenails and smoothed out my hard spots! Thank you for all the reminders about foods to eat & avoid! Carol U
In the past I was given biphosphinates and “forgotten”. Over 5 years went by and I wanted to get off. The Dr took me off and put me on Prolia. I demanded a second opinion but unfortunately they agreed with the first Dr. Under pressure, I took it for 1 1/2 yrs. A month after having a tooth pulled, my mouth increasingly developed painful sores. I t hurt to eat and to brush my teeth. I was misdiagnosed and given oral herpes meds which made me sick. Dr.gave me Magic Mouthwash which gave minimal relief. When I realized I had exposed bone protruding from jawbone inside my mouth I begged for a specialist. My Dr sent me to a dermatologist who was surprised the Dr sent me to see him and he sent me to an Ear nose throat Dr. After a CT scan I was sent to an oral surgeon who diagnosed Osteonecrosis of Jawbone and agreed very likely biphosphinates and Prolia were the cause. This was 9 months after stopping Prolia. I weighed under 90 lbs after all this and went to bed hungry due to mouth pain. I need to know 2 things. Will I continue to have fare ups when I bite my now deformed flesh under tongue, forever? And, is it true that if Prolia is stopped prematurely (whatever that means) the osteoporosis will BECOME more severe than it has ever been, negating all previous treatments. I am warning anyone I meet who mentions osteoporosis treatment of these dangers and I want to tell true facts. I’m now told I can break a bone simply turning over in bed and a list of things I cannot do . I refuse Osteoporosis Cinic I was told to attend may stop having dexa bone scans. I’m 77 and I’ve had enough bad advice. I bought a small rebounder( with out checking with any Dr first) I play music and bounce and have fun at last. I believe building muscles and balance will protect me better than any drugs – even if I didn’t suffer the side effect I had. Am I right?! Thanks for reading, I know it’s a long read. Carol
I’m heartbroken to learn that you’re yet one more victim of osteoporosis drugs, Carol! I can’t answer the question about your mouth, but I can share with you an article confirming that unfortunately when Prolia is stopped it can cause bones to weaken and fracture.
Here’s the link to the article that explains why that happens:
https://saveourbones.com/scientists-discover-why-stopping-prolia-increases-risk-of-fracture/
And you’re most certainly right about focusing on building muscle to strengthen your bones 🙂
You’re on the right track!
I had breast cancer last spring, my doctor put me on a drug called Letrozole 2,5mg to prevent the cancer to return. I took this med. for 3 months, but I had terrible side effects.
I suffer from osteoporosis and another side effect from this med. is bone fractures .
The doctor suggests I take Prolia injections, what I am afraid off . Next step is to try another drug for prevention for cancer to return. I don’t know what to do…
I’m sorry you have to be dealing with this, Charlotte! Here’s information on Prolia to help you decide how to proceed:
https://saveourbones.com/prolia-pros-and-cons/
https://saveourbones.com/this-works-better-than-osteoporosis-drugs/
https://saveourbones.com/scientists-discover-why-stopping-prolia-increases-risk-of-fracture/
And here’s an article to help you make the decisions:
https://saveourbones.com/who-should-you-trust/
Stay positive and healthy!
I took Fosamax for 1 year and stopped pretty much after I found your website. I have always tried to take care of my teeth to much success. I changed dentist (insurance) and she says I have beginning periodontal disease. Is it possible for that year to do “damage” to the bones around the teeth?
Thank you
Dear Sue,
We’re happy to provide you with an answer, so please check your email inbox within the next 24-48 hours.
In excellent health,
Customer Support
I always look forward to your comments and suggestions. Thank you.
You’re welcome!
Thank you, Ita.
You’re very welcome, Ita!